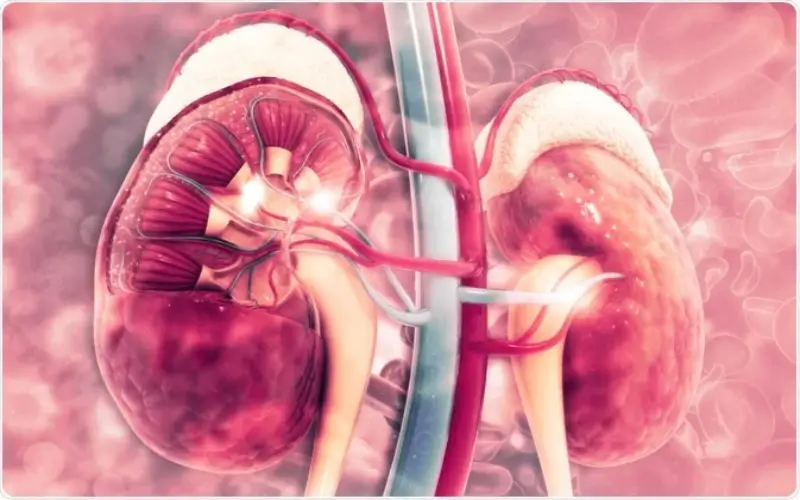
Stage 2 kidney disease is an early stage of chronic kidney disease (CKD) in which the kidneys show mild damage but still function relatively well. At this stage, the kidneys are working at about 60 to 89 percent of their normal capacity. Many people do not experience clear symptoms, which is why the condition is often discovered through routine blood or urine tests rather than obvious health problems.
The kidneys play a vital role in the body. They filter waste and excess fluids from the blood, balance electrolytes, regulate blood pressure, and help produce red blood cells. When kidney function begins to decline, these processes can slowly become less efficient. In Stage 2 kidney disease, the estimated glomerular filtration rate (eGFR) falls between 60 and 89, along with signs of kidney damage such as protein in the urine or structural abnormalities.
Common causes of Stage 2 kidney disease include diabetes and high blood pressure. Both conditions can damage the small blood vessels in the kidneys over time. Other causes may include kidney infections, autoimmune diseases, certain medications used for long periods, and a family history of kidney problems. Identifying and treating the underlying cause is important to prevent further damage.
Because symptoms are usually mild or absent at this stage, some people may only notice subtle changes. These can include slightly increased urination, mild swelling in the hands or feet, fatigue, or changes in urine appearance. However, many individuals feel completely normal. This makes regular health check-ups essential, especially for people at higher risk, such as those with diabetes, hypertension, or a family history of kidney disease.
Diagnosis typically involves blood tests to measure creatinine levels and calculate eGFR, along with urine tests to check for protein or blood. Imaging tests like ultrasound may also be used to look for structural changes in the kidneys. Early detection allows doctors to create a management plan to slow the progression of the disease.
Treatment for Stage 2 kidney disease focuses on controlling the underlying cause and protecting kidney function. Managing blood sugar levels in diabetic patients and keeping blood pressure within a healthy range are key steps. Doctors may prescribe medications such as ACE inhibitors or ARBs to help protect the kidneys. Lifestyle changes also play a major role. Eating a balanced diet low in salt and processed foods, maintaining a healthy weight, exercising regularly, and avoiding smoking can significantly reduce further damage.
It is also important to limit the use of over-the-counter pain relievers like nonsteroidal anti-inflammatory drugs (NSAIDs), which can strain the kidneys if used frequently. Staying well hydrated and following medical advice about protein intake can also support kidney health.
Stage 2 kidney disease does not usually require dialysis or advanced treatments, and many people can live normal lives with proper care. However, without management, the condition can progress to more serious stages over time. Regular monitoring through blood and urine tests helps track kidney function and ensures that any changes are addressed quickly.
Understanding Stage 2 kidney disease empowers individuals to take early action. With timely diagnosis, proper medical care, and healthy lifestyle choices, it is often possible to slow or even stop further progression and maintain good kidney function for many years.